“When I grow up, I’ll be a nurse to help you when you’re sick. I’ll do the nicest things for you to make you better quick.”
Shelia Swift, executive associate dean of academic affairs, recited that rhyme at career day when she was in kindergarten.
In the years since, she’s learned that being a nurse―and training the next generation of nurses―is not that poetically simple.
Nurses need knowledge. Skills perfected through practice. Real-world experience.
But beyond that, explains Dean Victoria Niederhauser, being a good nurse also requires a host of qualities that are difficult to teach in any traditional way.
“Nurses care for people in their worst moments. Small gestures, like reassuring words giving permission to feel afraid, frustrated, angry, mad, and sad, or therapeutic touch, like holding a hand, can ease the emotional turmoil of a difficult situation. We strive to teach our students the importance of proving safe and effective nursing care with empathy and compassion.”
Caring for people
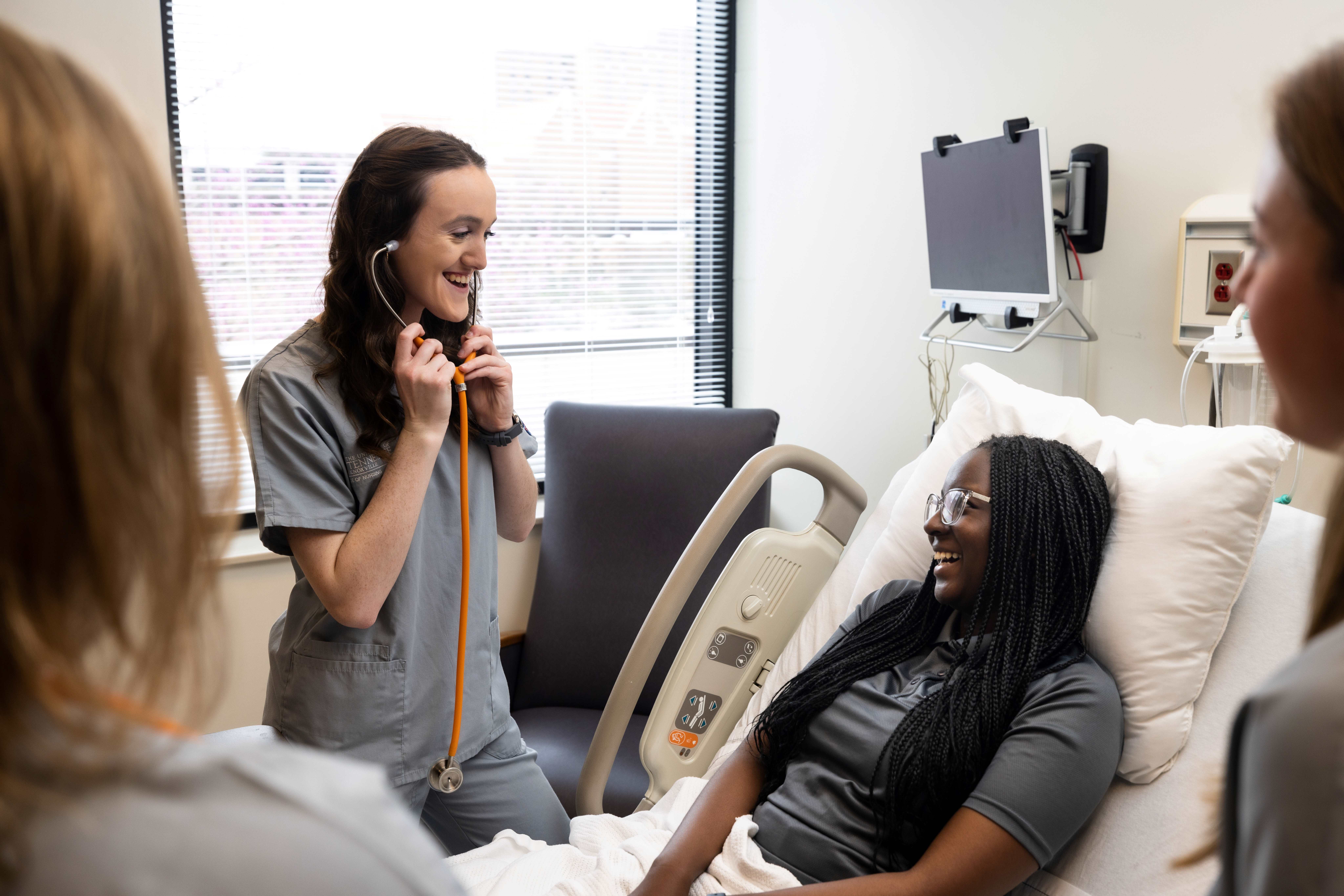
From the time they begin nursing classes in their junior year, UT nursing students spend a lot of time honing both their skills and empathic approach to caring. In the college’s various learning labs they encounter strategically devised scenarios that involve low-fidelity manikins (noncomputerized or capable of limited actions), high-fidelity manikins (computerized to mimic physiological responses), and standardized patients (actors working from scripts).
The newest lab, for the UT Medical Center Nursing Scholars, a new cohort of the traditional BSN program, will open this fall in the Innovation North facility at Cherokee Farms. Made possible through the collaborative partnership between UT and UTMC, the lab will house a 12-bed psychomotor skills lab and a four-bed high-fidelity lab that will look and feel like a hospital floor. The high-fidelity lab is where students and UTMC staff will practice routine and advanced medical–surgical care and support specialty skills from mother–baby care to critical care.
Susan Hébert, assistant dean of simulation, said the labs provide opportunities for nursing students to work through situations they may never encounter during their clinicals—such as a cardiac patient going into distress, a postpartum patient who begins to hemorrhage, or a patient having a schizophrenic episode. Students also experience interacting with people of diverse cultural backgrounds, sexual orientations, and temperaments.
Simulated practice helps students hone their medical skills. It also provides opportunities to practice interpersonal skills as they encounter challenging “patients” and their families and interact with other health care providers.
“We are committed to providing realistic and intentional learning experiences. In doing so, we provide students unique opportunities to challenge their critical thinking and ability to practice safely and communicate with empathy,” Hébert said.
Students’ sessions in the simulation labs are often video recorded so they can watch themselves at work, reflect on their performances, and think about what they’d do differently next time. Hébert said the simulation labs provide safe places where students can make mistakes and get second chances as they learn to think, talk, and interact like nurses.
UT’s simulation program is more extensive than those at many colleges and universities, and it is accredited by the Society for Simulation in Healthcare.
Hébert said the simulation spaces are also used by researchers to develop tools and applications that could revolutionize health care and health care education in the future.
Caring for the Community
Each semester during their junior and senior years, nursing students engage in at least 30 hours of academic service–learning at a community agency.
The college has 45 to 50 community partners, ranging from after-school programs to agencies that serve the poor and homeless to facilities that care for older adults. Students stay with their partner agencies for the duration, allowing them to build relationships.
“It’s a win-win-win,” Swift said. “Students are exposed to something that will enrich their professional nursing. It’s a win for the community partner because they have consistent help. And the clients benefit too.”
Swift said academic service-learning activities aren’t necessarily health related. And that’s OK, because students are learning soft skills like face-to-face verbal communication, time management, and problem-solving. By writing reflections about their service–learning, they also practice their written communication skills.
Students work in college programs like Vine School Health Center in Knoxville’s Vine Middle School, which provides health care to underserved children throughout Knox County, and the Precious Prints Project, which has provided more than 2,000 sterling silver fingerprint pendants to parents who have lost a child.
As associate dean of practice and global affairs, Professor Nan Gaylord oversees the Center for Nursing Practice, which encompasses both programs.
Gaylord helped found the Vine School Health Center in 1995. Now funded by federal grants and self-sustaining, the clinic logged more than 7,000 visits last year and saw students from every school in Knox County. College of Nursing faculty and two licensed clinical social workers staff the clinic. Undergraduates interested in pediatric nursing rotate through the clinic, working alongside the nursing staff.
The Precious Prints Program, a service project of the Student Nurses’ Association, is now operational in all Knoxville hospitals and in hospitals in several surrounding communities. There is an outreach effort to West Tennessee, and the program is being used as a model for a similar program in Las Vegas.
Gaylord said student nurses train hospital nurses in using Precious Prints kits and organize the annual Sprint for the Prints 5K, all of which helps student nurses gain empathy, bolster organizational skills, hone professionalism, and demonstrate leadership. Working with people in the community also helps them learn to prioritize, take responsibility, and recognize when they need to change tactics, raise a red flag, or ask for help.
“It teaches our students the characteristics we want them to develop as nurses,” she said.
Gaylord said caring for the underserved, whether it’s in the Knoxville area or halfway around the globe, also shows students that health care isn’t just care provided in the hospital.
“It’s fresh air, clean water, and access to health and prevention services, which make a difference in the health and well-being of our communities,” she said. “What we need to do as nurses is to provide care to our communities from a public health perspective.”
Caring for the World
During spring break 2023, recent graduate Margeaux Maerz traveled to Belize with a group of UT nursing students to do outreach and run health clinics with local providers.
“The Belize trip provided my first experience triaging and managing cases on a rolling basis,” Maerz said. “It was also a great opportunity to practice and hone my physical assessment skills. Learning to ask the right questions and the right follow-up questions to understand what the patient needed help with was crucial.”
The Belize trip is one of a growing number of international trips organized by the college to help students gain new perspectives on what it means to care for people around the globe.
Maerz attended UT as part of the Health Resources and Services Administration Nurse Corps Scholarship Program. Now that she’s graduated, she must work for two years at a hospital facing a critical staffing shortage. She’s currently serving as a nurse in the intensive care unit at Providence Alaska Medical Center in Anchorage, Alaska.
In another international experience, a group of nursing students went to Panama in January on a fact-finding mission funded by a grant from UT’s One Health Initiative―which seeks to improve local and global health by bringing together experts from various fields to find practical solutions to issues like food insecurity, loss of biodiversity, environmental contaminants, and substance abuse.
At the end of July, five students will travel to Nyeri, Kenya, where they will partner with WAKA Medical Training Institute and Hospital.
“They’ll be paired with one of their students and provide nursing care in the hospital with those other students for five days,” Gaylord said. “They’re going to be exposed to lots of things they haven’t been exposed to before.”
In August, three students will take an inaugural trip to Peru to work with a local agency that serves mountain people and teaches area women to provide minor health care when other medical care is unavailable. The students also will visit with a local traditional healer to learn health care customs.
Through international experiences, students learn how rudimentary health care can be in other places. They learn to slow down, have patience, communicate empathetically, and be creative and open-minded.
“They see that America doesn’t always have all the right answers to health care,” Gaylord said. “We have many, many resources that other countries don’t have, but Western medicine is only one way to take care of things.”
She said students also learn that health care often happens outside traditional hospitals and clinics.
For Maerz, who is just beginning her career, traveling to Belize showed her that nursing is both a science and an art: good nurses must possess traits well beyond their medical skills to care completely for their patients.
“This trip allowed me to appreciate the barriers to health that some populations face, and I realized that those barriers are not unique to Belize,” Maerz said. “Coming back to my clinical placement in the medical critical care unit at UTMC, I saw many of the same ailments and barriers to care—rural living, lack of transportation, mistrust of health care systems, poverty, and lack of health literacy, to name a few.”
—
CONTACT:
Kara Clark (865-974 9498, [email protected])







 Associate Professor Lisa C. Lindley has received a four-year award of $1.5 million from the National Institutes of Health National Institute of Nursing Research for her project “Effectiveness of Concurrent Care to Improve Pediatric and Family Outcomes at End of Life.” The study will investigate the impact of concurrent hospice care compared to standard hospice care in improving continuity and quality of pediatric end of life. Lindley will be working with an interdisciplinary team of pediatric end-of-life scholars from nursing, medicine, and health care economics to conduct the first-ever concurrent care study with children and adolescents in hospice care, using nationally represented Medicaid data from 2011 and 2013. The study will compare the effectiveness, potential burdens, and cost of concurrent care compared to standard hospice care for children and adolescents. The findings will expand our understanding of pediatric concurrent care and will inform clinicians and families of the value of this intervention for children and adolescents. This line of investigation is ultimately expected to improve care and outcomes for children, adolescents, and their families at end of life.
Associate Professor Lisa C. Lindley has received a four-year award of $1.5 million from the National Institutes of Health National Institute of Nursing Research for her project “Effectiveness of Concurrent Care to Improve Pediatric and Family Outcomes at End of Life.” The study will investigate the impact of concurrent hospice care compared to standard hospice care in improving continuity and quality of pediatric end of life. Lindley will be working with an interdisciplinary team of pediatric end-of-life scholars from nursing, medicine, and health care economics to conduct the first-ever concurrent care study with children and adolescents in hospice care, using nationally represented Medicaid data from 2011 and 2013. The study will compare the effectiveness, potential burdens, and cost of concurrent care compared to standard hospice care for children and adolescents. The findings will expand our understanding of pediatric concurrent care and will inform clinicians and families of the value of this intervention for children and adolescents. This line of investigation is ultimately expected to improve care and outcomes for children, adolescents, and their families at end of life. Associate Professor Sandra Mixer has received a four-year award of $2.6 million from the US Health Resources and Services Administration for her project “Transforming RN Roles in Community-Based Integrated Primary Care through Academic Practice Partnership.” The project supports the expansion of the academic practice partnership between the College of Nursing and Cherokee Health Systems (CHS), a nonprofit organization that provides primary care, behavioral health, and addiction services to more than 70,000 people throughout Tennessee. BSN students will be recruited and trained to provide integrated services to culturally diverse rural and underserved populations at four CHS sites in East Tennessee. The program includes both an innovative undergraduate nursing curriculum change and advancement of the RN workforce through professional development in primary and preventive care. It will provide the region’s first comprehensive community-based integrated primary care (CBIPC) training for students and RNs, with a focus on primary care, population health, and interprofessional education and practice and an emphasis on chronic disease prevention and control, recovery-based mental health and substance use, and childhood obesity. Faculty and clinical partnership liaisons and clinical coaches will serve as role models, preceptors, and mentors to students through more than 300 hours of clinical experiences in CBIPC teams over two years. Nursing workforce projections for the next decade forecast an unprecedented need for nurses to expand their roles in preventive, primary, and chronic care, and CBIPC training will uniquely qualify our BSN graduates to meet those challenges.
Associate Professor Sandra Mixer has received a four-year award of $2.6 million from the US Health Resources and Services Administration for her project “Transforming RN Roles in Community-Based Integrated Primary Care through Academic Practice Partnership.” The project supports the expansion of the academic practice partnership between the College of Nursing and Cherokee Health Systems (CHS), a nonprofit organization that provides primary care, behavioral health, and addiction services to more than 70,000 people throughout Tennessee. BSN students will be recruited and trained to provide integrated services to culturally diverse rural and underserved populations at four CHS sites in East Tennessee. The program includes both an innovative undergraduate nursing curriculum change and advancement of the RN workforce through professional development in primary and preventive care. It will provide the region’s first comprehensive community-based integrated primary care (CBIPC) training for students and RNs, with a focus on primary care, population health, and interprofessional education and practice and an emphasis on chronic disease prevention and control, recovery-based mental health and substance use, and childhood obesity. Faculty and clinical partnership liaisons and clinical coaches will serve as role models, preceptors, and mentors to students through more than 300 hours of clinical experiences in CBIPC teams over two years. Nursing workforce projections for the next decade forecast an unprecedented need for nurses to expand their roles in preventive, primary, and chronic care, and CBIPC training will uniquely qualify our BSN graduates to meet those challenges. Kim Powell joined the college in August as an assistant professor. She received her PhD along with a graduate certificate in health policy from the University of Tennessee, Knoxville, an MSN from Spalding University and a BSN from Purdue University.
Kim Powell joined the college in August as an assistant professor. She received her PhD along with a graduate certificate in health policy from the University of Tennessee, Knoxville, an MSN from Spalding University and a BSN from Purdue University.